Every treatment we rely on today had to begin somewhere. The painkiller you take for a headache, the vaccines that protect against serious diseases, even cutting-edge cancer therapies, all of them started as an idea. But before any of these reached pharmacies or hospitals, they had to be tested through clinical trials.
Clinical trials might sound complex, but at their core they are carefully designed studies that check if new treatments are safe and effective in real people. Without them, doctors would be left guessing about whether a therapy helps or harms.
So why do these trials matter so much, how do they shape the future of medicine, and what role do volunteers play? Let’s take a closer look.
Why Real-World Testing Matters
Many medical breakthroughs start in the lab. A scientist may identify a molecule that looks promising or a therapy that seems to work in animals. But what succeeds in a lab does not always succeed in people. The human body is more complex, and this is exactly why clinical trials are essential.
These studies are never casual experiments. They follow strict rules set by regulators like the FDA to ensure participant safety and reliable results. Without trials, we would have no filter to separate real progress from guesswork.
Think of trials as the bridge between discovery and daily care. They show whether a treatment that looks good on paper can actually help patients. And because modern trials strive to include people of different ages, genders, and backgrounds, the results better reflect the diversity of real-world populations.
From Idea to Treatment
Every potential therapy begins as a concept, maybe a drug that could block a virus or a treatment that could shrink a tumor. In the early stages, research happens in labs. Eventually, it must be tested in people.
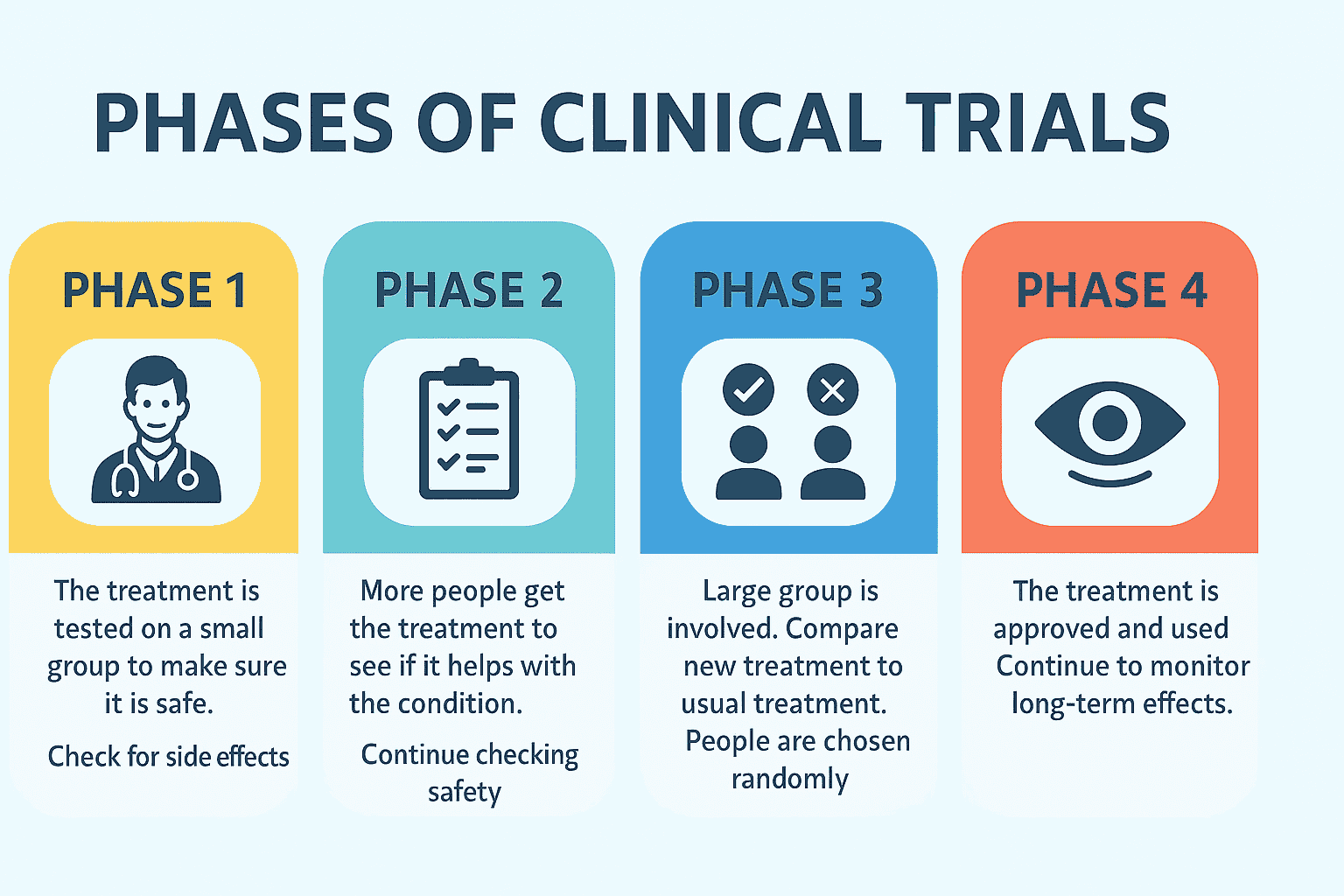
Clinical trials are how that testing happens. Each phase answers a different question: Is the treatment safe? Does it work as expected? What side effects appear? Who benefits most? To understand the basics of how trials are designed and conducted, you can read our earlier blog on what clinical trials are and how they work
The answers build layer by layer. When enough evidence shows a treatment is both safe and effective, regulators can approve it, and doctors can begin offering it to patients. It takes time, but that is what builds trust. By the time a therapy is available, it has been studied carefully and tested in real-world situations.
Taking On Rare Diseases and Global Threats
Not every trial focuses on common conditions. Some of the most important ones tackle rare diseases or urgent threats where no approved treatments exist.
For people living with rare conditions, a clinical trial may be the only chance to try a potential therapy. With more than 7,000 rare diseases identified and most still without approved treatments, trials often bring hope where few options exist.
We have also seen their importance during emergencies. During the COVID-19 pandemic, researchers and volunteers around the world worked together to test vaccines at record speed. Millions of lives were protected because so many stepped forward. Trials do not just shape the future of medicine, in the right moments, they save lives in the present.
The Role of Volunteers
Behind every trial are the people who choose to participate. Without volunteers, research simply cannot move forward.
Participants, whether they are living with a condition or perfectly healthy, help answer critical questions. Their experiences tell researchers how well a treatment works, what side effects it may cause, and who benefits most.
Not every volunteer sees personal benefits, though many do. Some gain early access to promising therapies, receive close medical monitoring, or have costs like travel covered. But beyond individual benefits, there is something greater: the knowledge that their involvement could help others in the future.
In many ways, trial participants are quiet heroes. Their willingness to contribute makes it possible for science to move from the lab to the clinic, turning ideas into care.
Moving Medicine Forward Together
Clinical trials are not only about data or regulations. They are about people and progress. They turn experimental science into real treatments, expand care for difficult conditions, and push healthcare toward greater inclusivity.
And at the heart of it all are the volunteers. People who give their time, share their experiences, and help researchers answer the toughest questions. Without them, new medicines and vaccines would remain ideas instead of becoming lifesaving solutions.
If you have ever wondered whether joining a trial might be right for you, or simply want to see what opportunities exist, you can explore studies on the DecenTrialz It is a straightforward way to discover what trials are available and how you might play a role in moving medicine forward.